Most people who get tennis elbow don't play tennis! In fact, less than 5% of all cases of tennis elbow occur in people who play tennis. Tennis elbow can happen to anyone who repeatedly uses their elbow, wrist, and hand for their job, sport, or hobby.
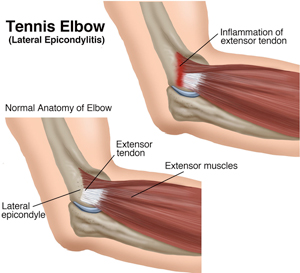
Tennis elbow is a painful condition caused by overuse of the "extensor" muscles in your arm and forearm, particularly where the tendons attach to rounded projections of bone (epicondyles) on the outside or lateral aspect of the elbow. The muscles you use to grip, twist, and carry objects with your hand all attach to the "lateral epicondyle" at the elbow. That's why a movement of the wrist or hand can actually cause pain in the elbow.
Prolonged use of the wrist and hand, such as when using a computer or operating machinery —and, of course, playing tennis with an improper grip or technique—can lead to tennis elbow. It can happen to athletes, non-athletes, children, and adults. It occurs more often in men than women, and most commonly affects people between the ages of 30 and 50.
Signs and Symptoms
Symptoms of tennis elbow can occur suddenly as a result of excessive use of the wrist and hand for activities that require force, such as lifting, twisting, or pulling. Forceful activities—like pulling strongly on a lawn mower starter cord—can injure the extensor muscle fibers and lead to a sudden onset of tennis elbow.
More commonly, though, symptoms of tennis elbow develop gradually over a period of weeks or months as a result of repeated or forceful use of the wrist, hand, and elbow. If you work as a grocery store cashier, you might have symptoms of tennis elbow as a result of repetitive (and often too forceful) typing—combined with continuous lifting of grocery bags.
Your symptoms may include:
Pain that radiates into your forearm and wrist
Difficulty doing common tasks, such as turning a doorknob or holding a coffee cup
Difficulty with gripping activities
Increased pain when you use your wrist and hand for lifting objects, opening a jar, or gripping something tightly, such as a knife and fork
Stiffness in the elbow
Weakness in the forearm, wrist, or hand
How Is It Diagnosed?
Tennis elbow usually occurs due to repeated movements. As a result, other muscles and joints in this region of the body may be affected as well. Your physical therapist will perform a careful examination not only of your elbow but of other areas of your body that might be affected and might be contributing to your pain. Your therapist will perform special manual tests that help diagnose the problem and help detect conditions such as muscle weakness that might have led to the problem in the first place. For instance, the therapist might ask you to gently tense or stretch the sore muscles to identify the exact location of the problem. Rarely is an x-ray required to diagnose this condition.
How Can a Physical Therapist Help?
The First 24 to 48 Hours
For the first 24 to 48 hours after acute onset of your pain, treatment includes:
Resting the arm by avoiding certain activities and modifying the way you do others
Using 10-20 minute ice treatments
Using elastic bandages or supports to take the pressure off of the painful muscles
Your physical therapist will decide if you should use a brace or support to protect your muscles while the area is healing. Depending on severity, your therapist may recommend that you consult with another health care provider for further testing or for consideration of additional treatment such as medication. In rare cases, treatments such as cortisone injection or surgery might be needed. Your physical therapist can help you determine whether you need a referral to another health care provider.
Your physical therapist can design a specific treatment program to speed your recovery. There will very likely be exercises and other treatments that you will be expected to do at home. Your physical therapist also might use special physical therapy treatments to help relieve pain, such as manual therapy, special exercises, and ice or heat treatments or both.
For an "acute" case of tennis elbow—one that has occurred within the past few weeks— it's important to treat as early as possible. Left untreated, tennis elbow may become chronic and last for months and sometimes even years. This is especially true if treatment is focused only on relieving pain and not on correcting the muscle weakness and bad habits that might have led to your condition in the first place.
Improve Your Ability to Move
Your physical therapist may use manual therapy to enable your joints and muscles to move more freely with less pain.
Improve Your Strength
Insufficient muscle strength can lead to tennis elbow. Sometimes the weakness is in the muscles of the wrist and forearm. In many cases, the problem stems from weakness of the supporting postural, or "core," muscles. In fact, you might find that it is necessary to improve your overall level of fitness to help manage your elbow condition. Based on the evaluation, your physical therapist can determine the type and amount of exercises that are right for you.
Physical therapists prescribe several types of exercises during recovery from tennis elbow:
Early in the treatment, when the pain is most intense, your therapist may recommend passive exercises in which your wrist and elbow are moved without the use of your muscles.
As your symptoms improve, you can move the wrist and elbow actively without assistance.
As the muscles become stronger and the symptoms have lessened, you will be able to begin using weights or resistance bands to further increase your strength. The amount of weight will need to be carefully monitored to make sure you continue to progress and avoid re-injuring your muscles.
Use Your Muscles the Right Way
Your physical therapist can help you retrain your muscles so that you use them properly. For example, when you lift a heavy grocery bag, you should contract the muscles around your shoulder blade and trunk to provide support for your arm muscles. This simple movement can be easily taught to you by a physical therapist can lessen the stress to the injured muscles and help you return to your normal activities while avoiding re-injury.
Return to Your Activities
Your physical therapist will help you remain active by teaching you how to modify your daily activities to avoid pain and further injury. Sometimes it's necessary to make changes at work, on the playing field, or in the home. Your physical therapist can help you make simple modifications to your work site, your computer set-up, your kitchen devices, your sports equipment, and even your gardening tools to lessen the strain to your hand, wrist, and forearm. Your therapist will emphasize the importance of taking stretch breaks so that your muscles get frequent rest from repetitive movements and standing or sitting in the same position.
Tennis may be a contributing factor to tennis elbow for several reasons. Sometimes the problem results from over-training. In other cases, the weight of the racquet or its grip may need to be adjusted. For others, the problem may stem from improper form, poor overall fitness, or a lack of strength in the supporting or "core" muscles of the trunk and shoulder blades. A physical therapist can help analyze the source of the problem and help find a solution.
Can this Injury or Condition be Prevented?
Yes! You can help prevent tennis elbow by staying fit, using proper technique in your sport or in your job, and using equipment that is well designed and appropriate for your body type and your level of activity. Your physical therapist can show you how. If you had tennis elbow years ago, you might be at risk for re-injury if the tendons did not have time to completely heal or if your muscle strength and joint mobility were not fully restored. Returning to sports or activities before you have fully recovered might result in an elbow that has persistent pain or is easily or frequently re-injured. A physical therapist can help determine when you are ready to return to your activities and sports and can help make sure that your elbow, forearm, and wrist are strong and ready for action.
Real Life Experiences
You work as a computer graphics engineer. Yesterday, you spent the day gardening with an electric lawn trimmer. This morning you woke up with pain and a feeling of stiffness on the outside of your elbow. The pain increases the more you move your elbow, forearm, and wrist. It also hurts to use your computer mouse or to pick up your coffee cup. You immediately schedule an appointment for an evaluation with a physical therapist. A physical therapist performs a full examination of your elbow and surrounding muscles and joints and can determine whether additional tests or referral to another health care provider is necessary. In most cases of tennis elbow, the therapist will manage your care through your full recovery.
This story was based on a real-life case. Your case may be different. Your physical therapist will tailor a treatment program to your specific case.
What Kind of Physical Therapist Do I Need?
All physical therapists are prepared through education and experience to treat a variety of conditions or injuries. You may want to consider:
A physical therapist who is experienced in treating people with musculoskeletal problems.
A physical therapist who is a board-certified clinical specialist or who completed a residency or fellowship in orthopaedics physical therapy. This therapist has advanced knowledge, experience, and skills that may apply to your condition.
You can find physical therapists who have these and other credentials by using Find a PT, the online tool built by the American Physical Therapy Association to help you search for physical therapists with specific clinical expertise in your geographic area.
General tips when you're looking for a physical therapist (or any other health care provider):
Get recommendations from family and friends or from other health care providers.
When you contact a physical therapy clinic for an appointment, ask about the physical therapists' experience in helping people with tennis elbow.
During your first visit with the physical therapist, be prepared to describe your symptoms in as much detail as possible, and say what makes your symptoms worse.
Further Reading
The American Physical Therapy Association (APTA) believes that consumers should have access to information that could help them make health care decisions and also prepare them for their visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of below-knee amputation. The articles report recent research and give an overview of the standards of practice both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
Weber C, Thai V, Neuheuser K, et al. Efficacy of physical therapy for the treatment of lateral epicondylitis: a meta-analysis BMC Musculoskelet Disord. 2015 Aug 25;16(1):223. Pubmed Abstract.
Shiri R, Viikari-Juntura E, Varonen H, Heliövaara M. Prevalence and determinants of lateral and medial epicondylitis: a population study. Am J Epidemiol. 2006; 164:1065-74. Pubmed Abstract.
Peterson M, Butler S, Eriksson M, Svärdsudd K. A randomized controlled trial of exercise versus wait-list in chronic tennis elbow (lateral epicondylosis). Ups J Med Sci. 2011; 116:269-79. PubMed Abstract. Publisher Full Text
*PubMed is a free online resource developed by the National Center for Biotechnology Information (NCBI). PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Reviewed by the MoveForwardPT.com editorial board.